50 YEARS OF ANTI-D
2018 marks the Fiftieth Anniversary of a discovery that ended the nightmare of RH disease for millions of women around the world.




The disease
Rh disease or hemolytic disease of the fetus and newborn (HDFN), is a blood disease that affects babies before they are even born. It can result in death before or shortly after birth as well as debilitating brain damage. Rh disease is caused by a mismatch of blood types. When a woman with “Rh Negative” blood becomes pregnant by a man who is “Rh Positive”, the fetus might also be Rh Positive. This can stimulate the mother’s immune system to produce defenses against what it takes to be “invaders”, the baby’s Rh+ red blood cells. Without prophylaxis, 24 million developing and newborn babies are at risk worldwide every year.(1,2)
1) Vinod K. Bhutani et al. Neonatal Hyperbilirubinemia and Rh Disease of the Newborn: incidence and impairment estimates for 2010 at regional and global levels.Pediatric Research Volume 74 | Number s1 | December 2013
2) Bowman JM. The prevention of Rh immunization. Transfus Med Rev.1988;2:129-150

A life changing discovery
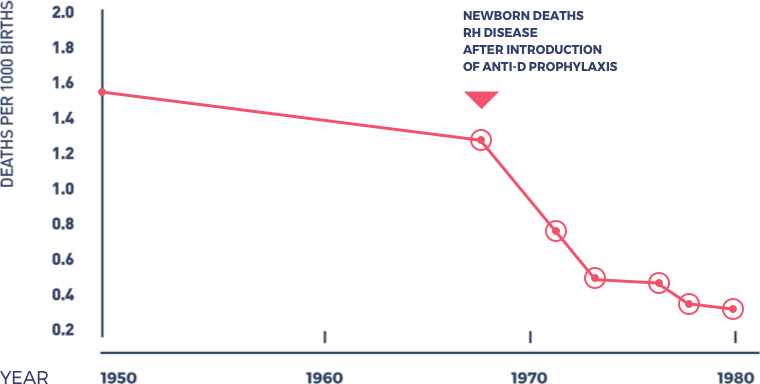
2018 marks the 50th anniversary of a discovery that has protected millions of pregnancies from HDFN and which has the potential to end this nightmare for virtually all women around theworld. In the 1960s HDFN was responsible for 10 percent of perinatal deaths in the U.S.2 , some 10,000 babies each year. Researchers at the Columbia Presbyterian Medical Center and Liverpool University helped develop Anti-D Immunoglobulin, the first effective prophylaxis to prevent HDFN. This breakthrough discovery was recognized by the 1980 Albert Lasker Award for Clinical Medical Research, sometimes referred to as “America’s Nobels”, given to Dr’s. John Gorman, Vincent Freda, William Pollack, Cyril Clarke and Ronald Finn
The Rhesus factor and the disease prevention
The transcript of a Witness Seminar held by the Wellcome Trust Centre for the History of Medicine at UCL.
London, on 3 June 2003 Edited by D T Zallen, D A Christie and E M Tansey

Today in the world
Although parents and children in more economically developed countries like the United States, Canada, Europe and Australia, are now safeguarded against this terrible threat by simple and relatively inexpensive injections, much of the world is still plagued by Rh Disease. In many countries, especially in Asia and Africa, the anti-d prophylaxis is still inaccessible to women who need protection. Failure to prevent Rh sensitization and to manage neonatal hyperbilirubinemia – a dangerous condition caused by HDFN – results in more than 100,000 avoidable neonatal deaths and many children with disabilities

The science behind the disease and its prevention
The main blood groups, A, B and O are followed by a “+” when the Rhesus protein (also known as the Rh or “d” protein) is present on red blood cells, and by a “-“ if it is not. So people with A+, B+ or O+ blood types are said to be Rh Positive and those with A-, B- or O- are Rh Negative. Neither condition has advantages or disadvantages, but when an Rh Negative woman becomes pregnant by an Rh Positive partner, there is a very good chance that the fetus will be Rh Positive like the father, and this can cause problems.2 Fetal blood will often make its way into the mother’s bloodstream – especially during childbirth. If the mother’s immune system detects the unknown Rh+ protein, it treats it as a threatening foreign substance and creates antibodies to destroy it. The formation of these antibodies takes some time and, since this tends to happen toward the end of the pregnancy, the first Rh + baby is generally not impacted. But once the mother’s immune system is “sensitized” to Rh+ blood cells and is armed with anti-d antibodies it will be ready to attack when they are again detected. Subsequent pregnancies with an Rh+ fetus are at deadly risk. The anti-D immunoglobulin developed in the 1960s changed all this. It is administered to the mother in the 28th week of her pregnancy and again just after delivery and prevents her immune system from becoming sensitized and developing the anti-D antibodies. Her next pregnancy will be protected